What you need to know about Type 2 Diabetes
What you need to know about Type 2 Diabetes
Type 2 diabetes is a common condition that causes the level
of sugar (glucose) in the blood to become too high.
Understanding
Type 2 Diabetes
According to studies 1, by 2030, diabetes will affect 5.5 million people in the United Kingdom. Type 2 diabetes affects approximately 90% of diabetics. Approximately 8% of patients with diabetes have Type 1 diabetes. About 2% of diabetics have the rarer forms of the disease.
Type 2 diabetes is a chronic medical condition marked by an increase in blood sugar (glucose) levels.
Glucose is transported from the bloodstream to the cells, where it is used as fuel, with the help of the hormone insulin. On the other hand, type 2 diabetes impairs the ability of your body’s cells to react to insulin as they ought to. Later on in the disease, your body might not produce enough insulin.
Uncontrolled type 2 diabetes can lead to chronically high blood glucose levels, which can lead to a number of symptoms as well as serious complications.
The World Health Organization provided the following data (WHO)2:
- Diabetes affected 8.5 percent of people worldwide in 2014.
- Only 4.7 percent of people in the world had diabetes in 1980.
- In 2016, 1.6 million deaths globally were directly attributable to diabetes.
- Adults with diabetes have a roughly threefold increased risk of heart attack and stroke.
- Kidney failure is frequently caused by diabetes.
What are the signs and
symptoms of type 2 diabetes?
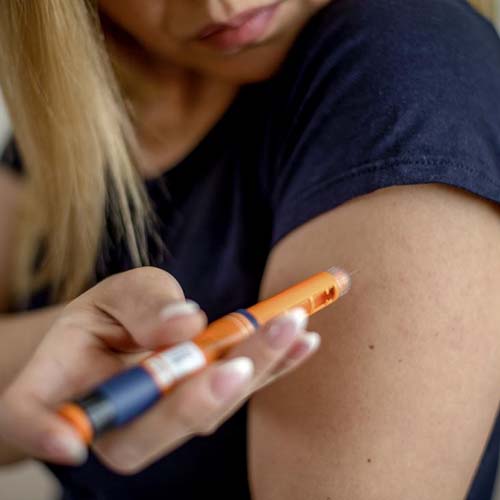
What are the signs and symptoms of type 2 diabetes?
If you have type 2 diabetes, your body cannot adequately use insulin to transport glucose into your cells. As a result, your tissues, muscles, and organs must rely on different energy sources. A variety of symptoms may be brought on by this sequence of actions.
It may take a while for type 2 diabetes to manifest. The symptoms may initially seem trivial and simple to ignore. Early signs and symptoms may include:
- Persistent hunger
- A lack of drive
- Fatigue
- Extreme thirst
- Urinating more often
- Hazy vision
- Numbness, tingling, or pain in your feet or hands
The symptoms become more severe as the disease advances, and they can lead to certain potentially hazardous complications.
Complications can arise if your blood glucose levels have been elevated for a long time:
- Problems with your eyes (diabetic retinopathy)
- Having neuropathy or experiencing numbness in your extremities
- Nephropathy (Kidney disease)
- Gum disease
- Heart attack or stroke
What Causes
Type 2 Diabetes?
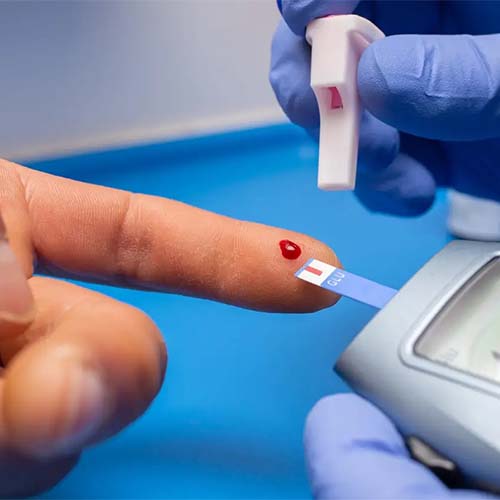
What Causes
Type 2 Diabetes?
The hormone insulin is produced naturally by the body. When you eat, your pancreas produces and releases it. Glucose is utilised as fuel by the body’s cells and is transferred from the bloodstream to the cells with the aid of insulin.
Your body becomes insulin resistant if you have type 2 diabetes. The hormone is no longer being used effectively by your body. Your pancreas will have to work harder to produce more insulin as a result of this.
Over time, this can injure the cells of your pancreas. It’s possible that your pancreas will finally stop producing any insulin.
If your body doesn’t produce enough insulin or doesn’t use it well, glucose builds up in your bloodstream. The cells in your body no longer have enough energy as a result. Doctors are unsure why this chain of events start. It can be related to pancreatic cell malfunction or cell signalling and control.
Although lifestyle choices are the main cause of type 2 diabetes, the following factors may increase your risk of being detected:
- Your family is genetically predisposed to having type 2 diabetes.
- Your family has a hereditary propensity for obesity, which can increase the risk of insulin resistance and diabetes.
- Your age is at least 45.
While your body’s resistance to insulin is the definitive cause of type 2 diabetes, there are usually a number of factors that raise your chances of developing that resistance.
How is type 2 diabetes
diagnosed?
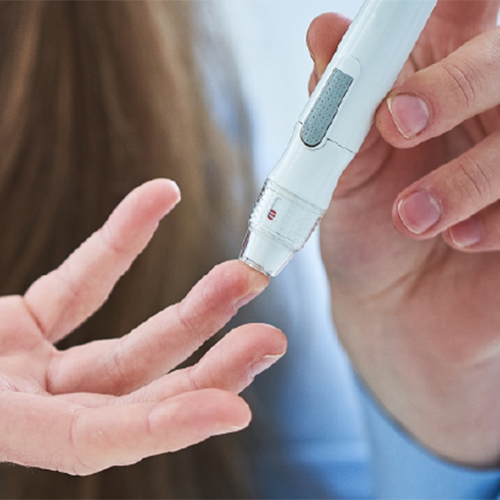
How is type 2 diabetes diagnosed?
If you suspect you have diabetic symptoms, regardless of whether you have prediabetes, you should see your doctor straight once. Blood tests can provide your doctor with a wealth of information. The following diagnostic tests may be used:
- A1C test for haemoglobin. The average blood glucose levels for the past two or three months are measured in this test. You don’t have to fast for this test, and the results can help your doctor diagnose you. A glycosylated haemoglobin test is another name for it.
- Glucose levels in the blood are measured after a period of fasting. This test determines the amount of glucose in your blood. It’s possible that you’ll need to fast for 8 hours before taking it.
- Test for oral glucose tolerance. Your blood is drawn three times during this test: before, one hour after, and two hours after you consume a glucose dose. The results of the test reveal how well your body handles glucose before and after the drink.
If you have diabetes, your doctor will provide you with advice on how to manage your condition, including:
- How to Self-Monitor Your Blood Glucose Levels
- Dietary recommendations
- Suggestions for physical activities
- Information on any medications you may require
It’s possible that you’ll need to consult an endocrinologist who specialises in diabetes therapy. To ensure that your treatment plan is working, you’ll probably need to see your doctor more frequently at first.
Risk factors & Complications for type 2 diabetes

Risk factors & Complications for type 2 diabetes
While some type 2 diabetes risk factors (including your age and family history, as mentioned above) are beyond of your control, certain lifestyle choices can greatly raise your risk of contracting the illness. Here are a few examples:
- Living with an excessive amount of weight. Being overweight increases your risk of having extra fatty tissue, which may make your cells more resistant to insulin.
- Adopting a more sedentary way of living. Your cells react better to insulin when you exercise.
- Consumption of a high-fat, high-processed diet. Highly processed meals frequently conceal sugar and refined carbs. If your lifestyle necessitates a more “grab-and-go” eating habit, talk to your doctor or a nutritionist about healthy substitutions.
You run a higher risk if you’ve ever had gestational diabetes or prediabetes, both of which are brought on by elevated glucose levels.
Complications associated with type 2 diabetes
Many people with type 2 diabetes can receive effective treatment. If left untreated, it can harm nearly all of your organs and result in serious problems, such as:
- Infections of the skin, such as bacterial or fungal infections
- Numbness and tingling in your limbs as well as digestive issues including vomiting, diarrhoea, and constipation might be brought on by nerve damage, commonly known as neuropathy.
- Your feet have a hard time healing from cuts or infections if you have poor foot circulation, which can eventually lead to gangrene and the need for a leg amputation.
- Hearing impairment
- Blurred vision, glaucoma, and cataracts can be caused by retinal damage, also known as retinopathy, and eye injury.
- Cardiovascular disorders include high blood pressure, arterial narrowing, angina, heart attacks, and strokes, for example.
- Women with diabetes are more likely to get a heart attack at a younger age than women without diabetes.
- Males with diabetes are 3.5 times more likely to experience erectile dysfunction (ED)
Hypoglycemia
Low blood sugar, or hypoglycemia, can happen. Some of the symptoms include shakiness, lightheadedness, and speech difficulties. Usually, you can solve this by consuming anything “quick-fix,” such as fruit juice, soft drinks, or hard sweets.
Hyperglycemia
Hyperglycemia can develop when blood sugar levels are excessively high. Increased thirst and frequent urination are its hallmarks. By constantly monitoring your blood glucose levels and being active, hyperglycemia can be prevented.
Complications during and after pregnancy
You must closely monitor your status if you have diabetes while expecting. Diabetes that isn’t well managed can lead to:
- Pregnancy, labour, and delivery are made more difficult
- Endangering your child’s developing organs
- Cause your baby to gain excessive weight
It may also increase the likelihood that your child may acquire diabetes in the future.
How is type 2
diabetes treated?

How is type 2 diabetes treated?
Type 2 diabetes can be controlled and even reversed in rare situations. Your doctor will inform you how often you should monitor your blood glucose levels as part of most treatment options. The objective is to stay within a certain range.
Your doctor will most likely recommend the following lifestyle adjustments to help you manage your type 2 diabetes:
- Consuming high-fibre and low-carbohydrate foods — fruits, vegetables, and whole grains can help maintain a constant blood glucose level.
- Eating on a regular basis
- Learning to pay attention to your body and quit eating when you’re satisfied
- Manage your weight and keep your heart healthy by avoiding processed carbohydrates, sweets, and animal fats as much as possible.
- To keep your heart healthy, get around half an hour of physical activity every day, exercise can also help you control your blood glucose levels.
Your doctor will show you how to spot the early signs of high or low blood sugar and what to do in each case.
Working with a dietitian can also help you figure out which foods will help you manage your blood sugar and which will make it unbalanced.
Insulin isn’t required for everyone with type 2 diabetes. If you do, it’s because your pancreas isn’t producing enough insulin on its own, and taking insulin as prescribed is critical. Other prescription drugs may also be beneficial.
Medications for type 2 diabetes
In some cases, lifestyle adjustments are sufficient to control type 2 diabetes. If not, there are a number of drugs that may be of assistance. These are a few of the drugs available:
- Metformin. This improves insulin sensitivity and lowers blood glucose levels. It serves as the initial line of treatment for the majority of type 2 diabetic patients.
- Sulfonylureas. These medications are taken orally and help the body produce more insulin. Insulin-secretagogues are another name for these medications. They influence the pancreas to release additional insulin. As a result, these medications are well known for resulting in hypoglycemia and weight gain. Sulfonylureas are among the most affordable medications and more effective than the majority of antidiabetic drugs.
- Meglitinides. These medications have a short half-life and stimulate the pancreas to make more insulin. The two most widely used medications in this family are nateglinide and repaglinide. These medications are best utilised in patients who are at risk of developing hypoglycemia, such as those with kidney illness, due to their short-acting nature.
- Thiazolidinediones. These improve the body’s sensitivity to insulin. The two medications that fall under this category are pioglitazone and rosiglitazone. These medications are contraindicated in people with heart failure and macular oedema and lead to fluid retention and weight gain.
- Inhibitors of the dipeptidyl peptidase 4 (DPP-4) enzyme. These less potent medications help to lower blood glucose levels. These medications work by lengthening incretins’ half-lives (GLP and GIP). They indirectly increase insulin sensitivity and glucose-dependent insulin secretion.
Since they do not result in hypoglycemia, these medications are referred to as euglycemic. However, they might intensify their effects and cause hypoglycemia if used along with sulfonylureas and insulin. Sitagliptin, Vildagliptin, and Linagliptin are DPP-IV inhibitors. Patients with hepatobiliary disease and those who have experienced pancreatitis in the past should abstain from using these medications. - Agonists for glucagon-like peptide-1. These aid in controlling blood sugar levels and delaying digestion. Liraglutide, Dulaglutide, and Semaglutide are among the medications in this class. Semaglutide is a brand-new GLP-1 analogue that is used to treat diabetes mellitus but is also linked to significant weight loss.
- Inhibitors of the sodium-glucose cotransporter-2 (SGLT2). These assist in the kidneys’ production of urine, which is used to remove sugar from the body. Because SGLT2 inhibitors work through the kidneys, they do not result in hypoglycemia. Dapagliflozin, empagliflozin, canagliflozin, and ertugliflozin are SGLT2 inhibitors. Some people using these medications may lose a lot of weight.
Each of the medications listed above has the potential to induce negative effects. Finding the optimal medicine or combination of medications to treat your diabetes may take some time for you and your doctor to figure out.
If your blood pressure or cholesterol levels aren’t where they should be, you might need to take medicine to address those issues as well.
Insulin therapy may be required if your body is unable to produce enough insulin. It’s possible that you’ll just require a long-acting injection at night, or that you’ll need to take insulin numerous times a day.
Learn about diabetes drugs that can help you manage your condition.
Diet & Managing
type 2 diabetes

Diet & Managing type 2 diabetes
Diet is a crucial tool for keeping blood glucose levels in a healthy range and your heart healthy.
The diet that is advised for those who have type 2 diabetes is the same diet that practically everyone should eat. All that’s left are a few crucial actions:
- Pick a variety of foods that are high in nutrients and low in empty calories.
- Be mindful of your portion sizes and try to stop eating when you are full.
- To calculate how much sugar or carbohydrates are in a serving size, carefully read the product labels.
Limit your intake of certain foods and beverages.
There are several meals and drinks you should avoid if at all possible if you have type 2 diabetes or even if you’re trying to prevent diabetes and reduce weight. Here are a few examples:
- Foods high in trans or saturated fats (like red meat and full-fat dairy products)
- Meat that has undergone processing (like hotdogs and salami)
- Margarine and shortening
- Baked goods that have undergone refinement (like white bread and cake)
- Snacks that are heavily processed and include a lot of sugar (packaged cookies and some cereals)
- Sweetened beverages (like regular soda and some fruit juices)
Your healthy lifestyle shouldn’t be derailed by a single meal, but it’s a good idea to talk to your doctor about dietary restrictions based on your blood sugar levels. Some people might require more frequent monitoring of their blood glucose levels after consuming these foods than others.
Foods to select
Just because you have type 2 diabetes doesn’t mean you can’t eat carbs. Healthy carbohydrates may provide you with energy and fibre. Some of the options include:
- Whole fruits
- Non-starchy vegetables (like broccoli, carrots, and cauliflower)
- Legumes, like beans
- Whole grains, like oats or quinoa
- Sweet potatoes
Eating fat is also not off-limits. Instead, choosing the right fats is crucial. The following foods contain omega-3 fatty acids:
- Tuna
- Sardines
- Salmon
- Mackerel
- Halibut
- Cod
- Flax seeds
Several foods include monounsaturated and polyunsaturated fats, including:
- Oils, such as olive oil
- Almonds, pecans, and walnuts.
- Avocados
Talk to your doctor about your specific nutritional goals. They could recommend that you consult a dietician who specialises in diabetes meals. If you collaborate, you may create a diet plan that is delicious and meets your lifestyle requirements.
Managing type 2 diabetes
Management of type 2 diabetes demands cooperation. Although you and your doctor will need to work closely together, the outcome will be greatly influenced by your decisions.
Your doctor might advise routine blood tests to monitor your blood glucose levels. This can let you assess how well you’re handling the circumstance. If you take medication, you can use these tests to learn how well it is working.
In addition, your doctor could advise you to check your blood sugar levels at home between visits using monitoring equipment. They’ll advise you on the frequency of use and the optimal range.
Your doctor may want to check your blood pressure and cholesterol levels because diabetes can raise your risk of cardiovascular disease. If you have heart disease symptoms, you may require more tests. An electrocardiogram (ECG or EKG) or a heart stress test are examples of these tests.
Including your family in the process may also be beneficial. They will be able to assist in an emergency if they are aware of the warning indications of blood glucose levels that are too high or too low.
Type 2 diabetes in children

Type 2 diabetes in children
According to Diabetes UK, about 7,000 children in the United Kingdom have type 2 diabetes. Around 40% of children with type 2 diabetes have no signs or symptoms and are diagnosed during routine physical examinations.
According to a 2016 study, the number of new occurrences of type 2 diabetes among teenagers has climbed to almost 5,000 each year. Another study from 2017 found a significant rise, especially among minorities and ethnic groupings.
If your child has been diagnosed with diabetes, their doctor will need to figure out if it is type 1 or type 2 before recommending a treatment plan.
You can help lower your child’s risk by encouraging them to eat healthily and be physically active every day, just as you can help adults manage or even reverse their type 2 diabetes diagnosis.
Summary

Summary
Type 2 diabetes is a disorder that occurs when glucose levels in the bloodstream become too high. It’s a frequent ailment that can be brought on by certain lifestyle choices. However, genetics, age, and family history can all enhance the chances of a diagnosis.
Certain lifestyle adjustments can help manage, and even reverse type 2 diabetes. Medication is provided for more serious situations.
If you have type 2 diabetes, talk to your doctor about building a treatment plan that fits your lifestyle. Because type 2 diabetes is so common, there are a variety of tools and first-hand accounts to assist you in managing, or breaking free from, the disease.

