Psoriatic arthritis (PsA)
Psoriatic arthritis (PsA)
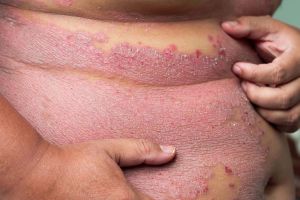
Psoriatic arthritis is a kind of arthritis that affects persons who have psoriasis, a skin ailment. It causes swollen, stiff, and painful joints in the affected joints.
Understanding Psoriatic arthritis (PsA)
Psoriatic arthritis is a kind of arthritis that affects persons who have psoriasis, a skin ailment. It causes swollen, stiff, and painful joints in the affected joints. Psoriatic arthritis, like psoriasis, is a chronic illness that can worsen over time. If the condition is severe, the joints may become permanently injured or distorted, necessitating surgery.
However, if psoriatic arthritis is detected and treated early on, it can be slowed down and permanent joint damage avoided or reduced.
In the United Kingdom, the prevalence of psoriatic arthritis is estimated to be between 0.1 and 0.3 percent of the overall population (50,000 to 156,000 people in England and Wales). It affects both men and women equally, with a peak in prevalence between the ages of 30 and 55.
Psoriatic arthritis (PsA)
Treatments

Psoriatic arthritis (PsA) Treatments
treatment modalities to treat the symptoms and ease chronic fibromyalgia pain.
PsA treatment aims to alleviate symptoms such as skin rashes and joint inflammation.
The “treat to target” method, which is based on a person’s specific preferences, was recommended in 2018 guidelines. After determining a precise treatment objective and how to track progress, a doctor collaborates with you to choose treatments.
There are numerous therapy choices available to you. One or more of the following may be included in a standard treatment plan:
Nonsteroidal anti-inflammatory drugs (NSAIDs)
These drugs help to reduce joint discomfort and swelling. Ibuprofen (Advil) and naproxen are two over-the-counter (OTC) choices (Aleve). If over-the-counter remedies don’t work, your doctor may prescribe NSAIDs in greater doses.
NSAIDs can produce the following side effects if used incorrectly:
- Stomach irritation
- Stomach bleeding
- Heart attack
- Stroke
- Liver and kidney damage
Disease-modifying antirheumatic drugs (DMARDs)
Apremilast (Otezla) is a newer orally administered DMARD. It operates by inhibiting the enzyme phosphodiesterase 4, which is implicated in inflammation.
The following are some of the DMARD adverse effects:
- Liver damage
- Bone marrow suppression
- Lung infections
Biologics
Psoriatic illness is now treated with five different types of biological medicines. They’re divided into groups based on what they target and suppress (block or diminish) in the body:
- Tumour necrosis factor-alpha (TNF-alpha) inhibitors:
- Adalimumab (Humira)
- Certolizumab (Cimzia)
- Golimumab (Simponi)
- Etanercept (Enbrel)
- Infliximab (Remicade)
- Interleukin 12 and 23 (IL-12/23) inhibitors:
- Ustekinumab (Stelara)
- Interleukin 17 (IL-17) inhibitors
- Secukinumab (Cosentyx)
- Ixekizumab (Taltz)
- Interleukin 23 (IL-23) inhibitors
- Guselkumab (Tremfya)
- T-cell inhibitors
- Abatacept (Orencia)
Biologics are given as an injection under the skin or as an IV infusion. Because these drugs suppress your immune system, they can put you at risk for dangerous infections. Nausea and diarrhoea are two more common adverse effects.
Steroids
Immunosuppressants
Medications like azathioprine (Imuran) and cyclosporine (Gengraf) help to slow down the excessive immune response in people with PsA, especially when it comes to psoriasis symptoms. Now that TNF-alpha inhibitors are accessible, they aren’t utilised as frequently. Immunosuppressants might make you more susceptible to infections by weakening your immune system.
Topical treatments
The irritating PsA rash can be relieved with creams, gels, lotions, and ointments. These treatments are both over-the-counter and prescription-only.
Among the possibilities are:
- Anthralin
- Calcitriol or calcipotriene, which are forms of vitamin D-3
- Salicylic acid
- Steroid creams
- Tazarotene, which is a derivative of vitamin A
Light therapy and other PsA medications
To treat psoriasis skin rashes, light treatment involves taking medicine and then being exposed to intense light.
PsA symptoms can also be treated with a few additional drugs. Secukinumab (Cosentyx) and ustekinumab are two of them (Stelara). These medications are injected beneath your skin. Stelara comes with a warning that it can make you more susceptible to infections and cancer.
What are the
symptoms of
Psoriatic arthritis (PsA)
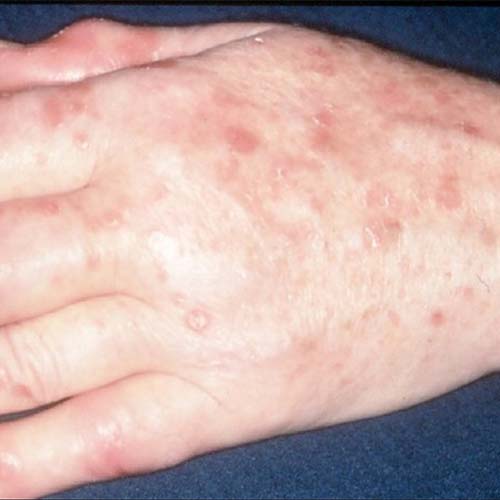
What are the symptoms of
Psoriatic arthritis (PsA)
PsA symptoms vary from individual to person. They might range in severity from minor to severe. Your ailment may go into remission at times, and you will feel better for a while. Your symptoms may worsen at other times. The type of PsA you have affects your symptoms as well.
The following are some of the most common PsA symptoms:
- Swollen, tender joints on one or both sides of your body
- Morning stiffness
- Swollen fingers and toes
- Painful muscles and tendons
- Scaly skin patches, which may get worse when joint pain flares up
- Flaky scalp
- Fatigue
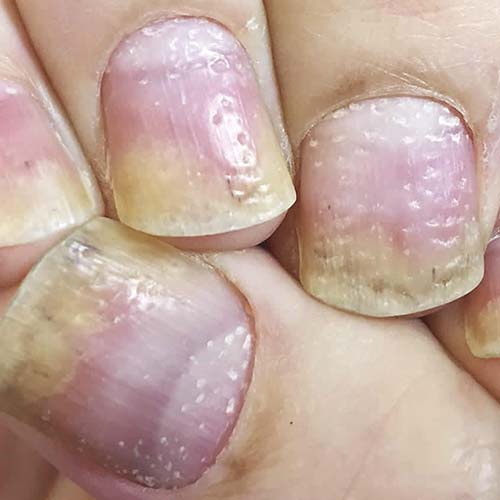
- Nail pitting
- Separation of your nail from the nail bed
- Eye redness
- Eye pain (uveitis)
Spondylitis PsA, in particular, might present with the following signs and symptoms:
- Spinal pain and stiffness
- Pain, weakness and swelling in your:
- Hips
- Knees
- Ankles
- Feet
- Elbow
- Hands
- Wrists
- Other joints
- Swollen toes or fingers
Five or more joints on both sides of your body are affected by symmetric PsA. PsA affects fewer than five joints asymmetrically, however, they can be on opposite sides.
Psoriatic arthritis mutilans is a rare type of arthritis that causes joint deformation. It has the potential to shorten the fingers and toes of those who are affected. Pain and swelling in the end joints of your fingers and toes are symptoms of distal PsA.
What Causes & Triggers
Psoriatic arthritis (PsA)

What Causes & Triggers
Psoriatic arthritis (PsA)
What causes psoriatic arthritis?
PsA is a disease that runs in families. Psoriatic arthritis affects nearly one-third of patients with psoriasis.
It usually appears 5 to 10 years after psoriasis is diagnosed, though some people may experience joint pain before noticing any skin symptoms.
For people who have a tendency to acquire PsA, something in the environment generally starts the disease. It could be a sickness, a stressful situation, or an injury. Psoriatic arthritis, like psoriasis, is thought to be caused by the immune system wrongly attacking healthy tissue.
However, why some people with psoriasis develop psoriatic arthritis while others do not is unknown.
What can trigger a psoriatic arthritis flare-up?
Flare-ups of PsA make the situation worse for a while. PsA flares can be triggered by a variety of factors. Triggers fluctuate from person to person.
Keep a symptom record to learn your triggers. Write down your symptoms and what you were doing when they first appeared each day. Make a note of any changes to your regimen, such as if you started taking a new prescription.
The following are some of the most common PsA triggers:
- Infections, like strep throat and upper respiratory infections
- Injuries, like a cut, scrape, or sunburn
- Dry skin
- Stress
- Cold, dry weather
- Smoking
- Heavy drinking
- Stress
- Excess weight
- Medications, like lithium, beta-blockers, and antimalarial drugs
While you won’t be able to avoid all of these triggers, you can try to manage stress, quit smoking, and limit your alcohol consumption.
Ask your GP whether you’re taking any medications that have been linked to the onset of PsA symptoms. If this is the case, you might consider switching to a different medication.
How is
Psoriatic arthritis (PsA)
diagnosed?
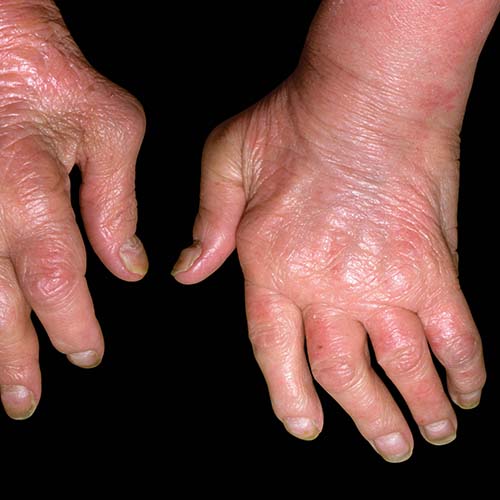
How is Psoriatic arthritis (PsA) diagnosed?
A GP may ask you to complete a questionnaire to assist them in determining whether or not you require a referral. Every year, people with psoriasis should be asked to complete this survey.
If your doctor suspects you have psoriatic arthritis, they should refer you to a rheumatologist (a joint expert) for an evaluation.
If you have psoriasis and joint pain, a rheumatologist will most likely be able to diagnose psoriatic arthritis. Other types of arthritis, such as rheumatoid arthritis and osteoarthritis, will be ruled out.
With imaging and blood testing, your doctor must rule out other causes of arthritis, such as RA and gout, before diagnosing PsA. These imaging examinations check for damage to joints and other tissues, and they include the following:
- X-rays – These check for inflammation and damage to bones and joints. This damage is different in PsA than it is in other types of arthritis.
- MRIs – Radio waves and strong magnets make images of the inside of your body. These images can help your doctor check for joint, tendon, or ligament damage.
- CT scans and ultrasounds – These can help doctors determine how advanced PsA is and how badly joints are affected.
Blood testing for these compounds can help you figure out if you have any inflammation in your body:
- C-reactive protein – This is a substance your liver produces when there’s inflammation in your body.
- Erythrocyte sedimentation rate – This reveals how much inflammation is in your body. But it can’t determine if the inflammation is from PsA or other possible causes.
- Rheumatoid factor (RF) – Your immune system produces this autoantibody. It’s usually present in RA but negative in PsA. An RF blood test can help your doctor tell whether you have PsA or RA.
- Joint fluid – An arthrocentesis removes a small amount of liquid from your knee or other joints. If uric acid crystals are in the fluid, you might have gout instead of PsA. A culture fluid test can rule out infection or sepsis.
- Red blood cells – A low red blood cell count from anaemia is common in people with PsA.
There is no single blood or imaging test that can indicate whether or not you have PsA. To rule out other possible causes, your doctor performs a series of tests.
Hyperbaric oxygen therapy
Accumulated data show that Hyperbaric oxygen therapy (HBOT) has anti-inflammatory effects and other positive influences on the immune system, making it a rational treatment in the management of psoriasis plaques.
Cryotherapy
Cryotherapy can be used in therapeutic treatments to target plaques of psoriasis. Whole-body cryotherapy may also help offer relief to psoriasis symptoms. One study found that 72 percent of patients saw their psoriasis plaques clear up after a cryotherapy treatment.
Ozone therapy
Ozone therapy can attenuate local inflammatory reactions and the activation of Th17 cells in psoriasis by inhibiting the NF-κB pathway. Our results show that ozone therapy is effective in treating psoriasis.
Red Light Therapy
Infrared Sauna therapy
Infrared sauna therapy provides a non-invasive, relaxing and refreshing approach to soothe itchy, sore, dry and reddened skin to help manage the symptoms of skin conditions including eczema and psoriasis.
IV DRIP THERAPY

Hyperbaric oxygen therapy
Accumulated data show that Hyperbaric oxygen therapy (HBOT) has anti-inflammatory effects and other positive influences on the immune system, making it a rational treatment in the management of psoriasis plaques.

Cryotherapy
Cryotherapy can be used in therapeutic treatments to target plaques of psoriasis. Whole-body cryotherapy may also help offer relief to psoriasis symptoms. One study found that 72 percent of patients saw their psoriasis plaques clear up after a cryotherapy treatment.

Ozone therapy
Ozone therapy can attenuate local inflammatory reactions and the activation of Th17 cells in psoriasis by inhibiting the NF-κB pathway. Our results show that ozone therapy is effective in treating psoriasis.

Red Light Therapy

Infrared Sauna therapy
Infrared sauna therapy provides a non-invasive, relaxing and refreshing approach to soothe itchy, sore, dry and reddened skin to help manage the symptoms of skin conditions including eczema and psoriasis.
IV DRIP THERAPY
Psoriatic arthritis (PsA)
Types
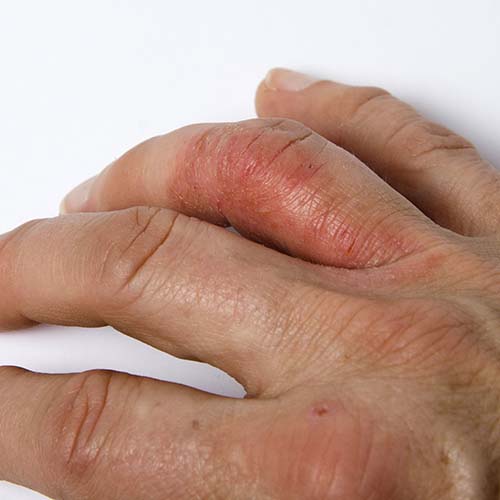
Psoriatic arthritis (PsA) types
There are five different kinds of PsA.
Symmetric PsA
This type of arthritis affects the same joints on both sides of the body, such as your left and right knees. Symptoms are similar to rheumatoid arthritis (RA).
Symmetric PsA is less severe than RA and causes less joint deformity. However, symmetric PsA can be debilitating. This form affects almost half of all patients with PsA.
Asymmetric PsA
One or more joints on one side of your body are affected. Your joints may become swollen and inflamed. The symptoms of asymmetric PsA are usually modest. It affects around 35% of people with PsA.
Distal interphalangeal predominant PsA
The joints nearest to your nails are involved in this type. The distal joints are what they’re called.
Spondylitis PsA
Your spine is involved in this sort of PsA. Your entire spine could be impacted, from your neck to your lower back. The movement might be quite uncomfortable as a result of this. It’s possible that your hands, feet, legs, arms, and hips will be impacted.
Psoriatic arthritis mutilans
This is a deforming and severe variant of PsA. This type affects about 5% of those with PsA. The hands and feet are commonly affected by psoriatic arthritis mutilans. It might also make your neck and lower back hurt.
Diet & natural
remedies

Diet & natural remedies
Is it possible to reduce the symptoms of psoriatic arthritis by changing your lifestyle?
If you can, incorporate exercise into your regular regimen.
Limit alcohol and quit smoking
Smoking is harmful to both your joints and the rest of your body. To help you quit, talk to your doctor about counselling, medicine, or nicotine replacement.
Limit your alcohol consumption as well. Some PsA drugs may interact with it.
Relieve stress
Tension and stress can aggravate arthritis flare-ups. To relax your mind and body, meditate, practise yoga, or try other stress-relieving practises.
Use hot and cold packs
Muscle soreness can be relieved with warm compresses and hot packs. Cold packs can also help to relieve joint pain.
Move to protect your joints
Instead of using your fingers, use your body to open doors. With both hands, lift large objects. To open jar lids, use jar openers.
Consider natural supplements and spices
Anti-inflammatory effects are found in omega-3 fatty acids. These good fats, which can be found in a variety of supplements, help to reduce joint inflammation and stiffness.
While studies suggest that supplements may have health advantages, the Food and Drug Administration (FDA) does not regulate supplement purity or quality. Before you start using supplements, you should consult your doctor.
Turmeric is a powerful spice with anti-inflammatory characteristics that may help reduce inflammation and PsA flare-ups. Turmeric can be used in a variety of dishes. Some people use it as a substitute for golden milk in tea or lattes.
Psoriatic arthritis diet
While there is no single food or diet that may treat PsA, a nutrient-dense, well-balanced diet can help reduce inflammation and alleviate symptoms. Changes to your diet that are beneficial to your joints and body will pay you in the long run.
In a nutshell, increase your intake of fresh fruits and vegetables. They aid in the reduction of inflammation as well as weight management. Excess weight puts further strain on already strained joints. Sugar and fat, both of which are inflammatory, should be avoided. Healthy fats, such as fish, seeds, and nuts, should be prioritised.
What are the
stages of
Psoriatic arthritis?

What are the stages of Psoriatic arthritis?
Psoriatic arthritis (PsA) has a different route for each person who is diagnosed with it. Some people may simply have minor symptoms and have a minimal joint impact. Others may have joint deformities and bone growth in the future.
It’s unclear why some people’s condition progresses more quickly while others don’t. Early diagnosis and therapy, on the other hand, can assist to alleviate discomfort and slow joint degeneration. It’s critical to consult your doctor as soon as you notice indications or symptoms that could indicate Psoriatic arthritis.
Early-stage PsA
You may notice modest symptoms such as joint swelling and limited range of motion in the early stages of this arthritis. These symptoms may appear concurrently with the onset of psoriasis skin lesions or years later.
The most common treatment is NSAIDs. These drugs help with pain and symptoms, but they don’t stop PsA from progressing.
Moderate PsA
Depending on the type of PsA you have, symptoms will likely develop in the intermediate or medium stages, necessitating more advanced treatments such as DMARDs and biologics. These drugs can help you feel better. They may also assist to slow the progression of harm.
Late-stage PsA
Bone tissue is severely compromised at this point. Bone growth and joint deformities are likely. The goal of treatment is to alleviate symptoms and prevent consequences from escalating.
Psoriatic arthritis (PsA)
Risk Factors
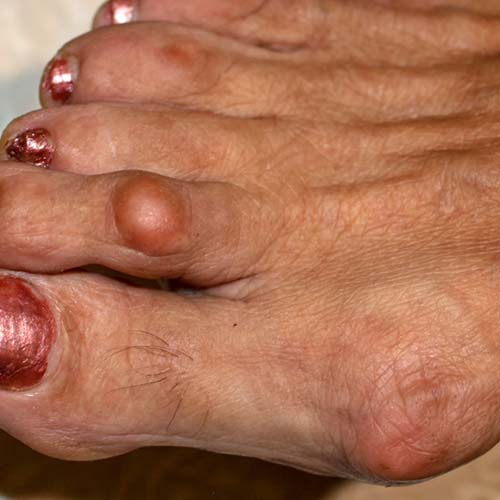
Psoriatic arthritis (PsA) Risk Factors
If you do any of the following, you’re more likely to get PsA:
- Have psoriasis
- Have a parent or sibling who suffers from PsA?
- Are between 30 and 50 years old (though children can get it, too)
- Has contracted strep throat
- Has contracted HIV
Psoriatic arthritis puts you at risk for a variety of problems, including:
- Psoriatic arthritis mutilans
- Difficulties with the eyes, such as conjunctivitis or uveitis
- Coronary heart disease
Psoriatic arthritis
vs.
rheumatoid arthritis
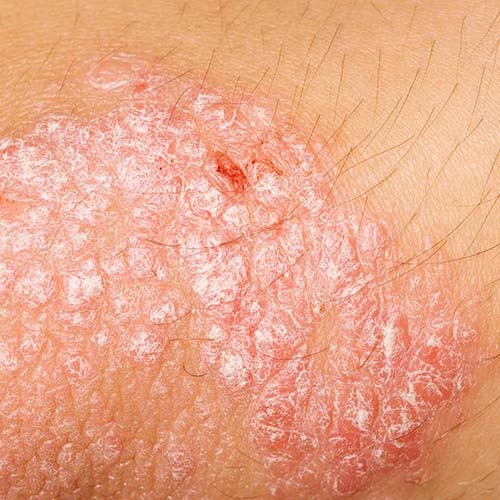
Psoriatic arthritis vs. rheumatoid arthritis
There are various kinds of arthritis, including PsA and RA. While they may have the same name and many of the same symptoms, they are caused by different underlying reasons.
Psoriatic arthritis is produced by psoriasis patients. This is a skin ailment that results in lesions and scaly patches on the surface of the skin.
RA is a type of autoimmune disease. It happens when the body attacks the tissues that line the joints by accident. This results in swelling, discomfort, and eventually joint damage.
PsA affects men and women roughly equally, but women are more likely to develop RA. For most people, PsA first appears between the ages of 30 and 50. RA commonly appears later in life, around middle age.
Both Psoriatic arthritis and Rheumatoid arthritis have several symptoms in common in their early stages. Pain, oedema, and joint stiffness are some of the symptoms. It may become evident which ailment you have as the symptoms grow.
Thankfully, a doctor won’t have to wait for arthritis to worsen before diagnosing it. Blood and imaging tests might help your doctor figure out what’s wrong with your joints.
Psoriatic arthritis (PsA)
Summary
Psoriatic arthritis (PsA) Summary
Everyone has a unique perspective. Some folks have relatively minor symptoms that only present issues on occasion. Others have symptoms that are more severe and incapacitating.
PsA will have a greater impact on your ability to move around the more severe your symptoms are. Walking, climbing stairs, and doing other daily tasks may be difficult for people with a lot of joint injuries.
The following events will have an impact on your outlook:
- You received a diagnosis of PsA at a young age.
- Your condition was severe when you got your diagnosis.
- A lot of your skin is covered in rashes.
- A few people in your family have PsA.
Follow your doctor’s therapy recommendations to improve your perspective. It’s possible that you’ll have to try several drugs to discover the one that works best for you.