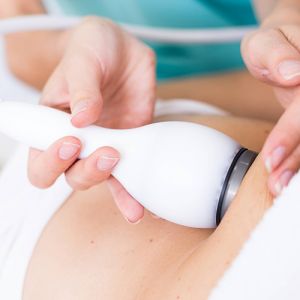
Rheumatoid Vasculitis
Rheumatoid Vasculitis
Rheumatoid vasculitis is an inflammation of the blood vessels caused by rheumatoid arthritis. It occurs in certain persons with rheumatoid arthritis (RA) who have had it for a long period. Rheumatoid arthritis (RA) is an autoimmune illness. An issue with the immune system causes an autoimmune disease. The immune system’s job is to keep the body healthy and free of disease.
Understanding Rheumatoid Vasculitis
Rheumatoid vasculitis is an inflammation of the blood vessels caused by rheumatoid arthritis. It occurs in certain persons with rheumatoid arthritis (RA) who have had it for a long period.
Rheumatoid arthritis (RA) is an autoimmune illness. An issue with the immune system causes an autoimmune disease. The immune system’s job is to keep the body healthy and free of disease. It accomplishes this by targeting potentially harmful substances in the body, like viruses. Your immune system assaults your own body when you have an autoimmune disease.
The joints are frequently the first to be affected by RA. Rheumatoid vasculitis develops when it affects your blood vessels. Blood is carried throughout the body through blood vessels. They transport oxygen-rich blood from the heart to the body and oxygen-depleted blood back to the heart.
Small and medium-sized blood vessels can be affected by rheumatoid vasculitis. Except in rare situations, it has no effect on big blood arteries. Blood vessels can get blocked as a result of damage. This can result in a lack of oxygen reaching some sections of the body. This can result in tissue damage or death.
Only one form of vasculitis exists rheumatoid vasculitis. There is a variety of them. Other autoimmune illnesses, such as lupus, can cause vasculitis. It can also happen on its own.
RA affects millions of people. It mostly affects women in their 40s and 60s. Rheumatoid vasculitis affects just a small percentage of RA patients. Rheumatoid vasculitis is more common in men than in women with RA. Because of better RA therapies, it may be less common than it once was.
What are the signs and
symptoms of
Rheumatoid Vasculitis?
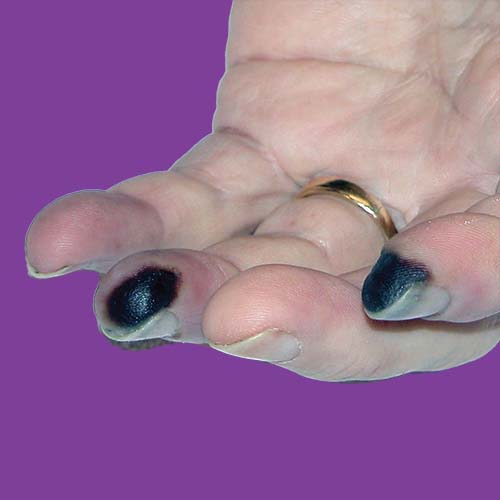
What are the signs and symptoms of Rheumatoid Vasculitis?
Symptoms may not appear for several years after you’ve had RA for 10 years or more. They usually begin after your joint illness has become less active for a while.
Rheumatoid vasculitis affects blood vessels throughout the body. As a result, it can induce a wide range of symptoms. Blood vessels in the skin, fingers and toes, nerves, eyes, and heart are the most commonly affected. This lowers blood flow to these areas, causing them to deteriorate.
Tiredness, fever, and weight loss are common symptoms in persons with rheumatoid vasculitis. These symptoms are also frequent in RA. People with rheumatoid vasculitis, on the other hand, frequently have them in a more severe form. Other rheumatoid vasculitis symptoms include:
- Skin sores (ulcers)
- Purplish bruises
- Pain in fingers and toes
- Tissue death (gangrene) in fingers and toes
- Muscle weakness in parts of the body
- Loss of feeling in parts of the body
- Tingling and pain in parts of the body
- Eye pain
- Eye redness
- Blurry vision
- Chest pain
- Abnormal heart rhythms, some of which may be fatal
What Causes
Rheumatoid Vasculitis?
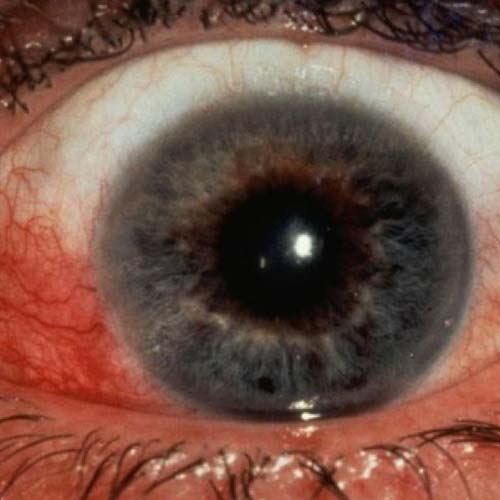
What Causes Rheumatoid Vasculitis?
Researchers are unable to explain what causes rheumatoid vasculitis. The immune system is a complicated mechanism. Rheumatoid vasculitis is caused by a variety of factors. Genes are more likely to blame.
How is
Rheumatoid Vasculitis
diagnosed?
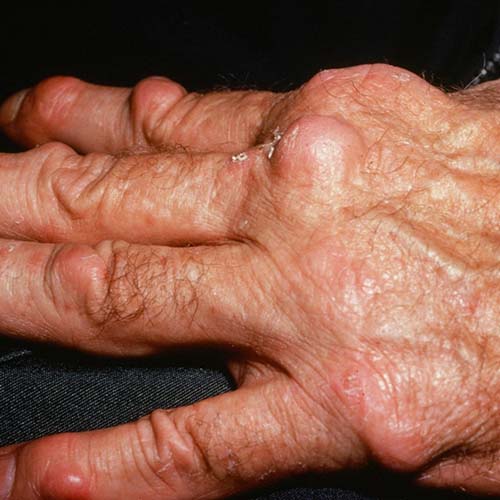
How is Rheumatoid Vasculitis diagnosed?
Your healthcare professional will check you for rheumatoid vasculitis and other problems if you have RA. Your healthcare professional will inquire about your medical history as well as your current symptoms. You’ll also be subjected to a physical examination. Your doctor will run tests to make sure your symptoms aren’t the result of another type of vasculitis or another health problem. These tests may involve the following:
- Blood tests to check for inflammation
- Blood cultures to look for infection
- Biopsy of a blood vessel
- Angiography to look at a blood vessel
Other tests may be required to check for harm to the bodily parts serviced by the damaged vessels. You might need an electrocardiogram (ECG) to check your heart rhythm, for example.
What are the risks &
preventative Factors
of rheumatoid vasculitis?
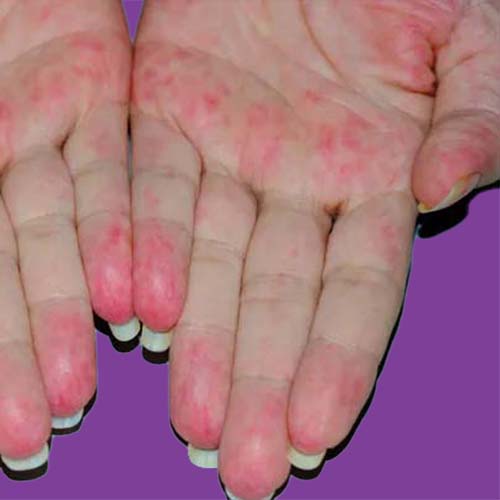
What are the risks & preventative Factors of rheumatoid vasculitis?
If you’ve had severe RA for a long period, you may be at higher risk for rheumatoid vasculitis. Smoking may also put you at a higher risk.
You might be able to lower your risk of rheumatoid vasculitis if you treat your RA early and aggressively. Stopping Smoking may also help lower your risk.
What is the treatment
options for
rheumatoid vasculitis?
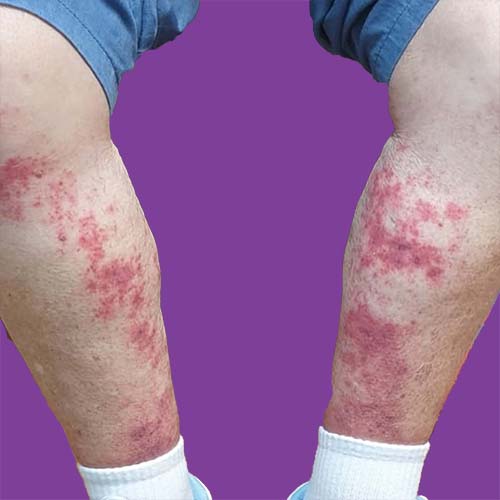
What is the treatment options for rheumatoid vasculitis?
Depending on the severity of the vasculitis and which blood vessels are involved, your treatment may differ. Rheumatoid vasculitis has no known cure. Early treatment, on the other hand, can help reduce vessel damage and alleviate symptoms.
If you only have modest rheumatoid vasculitis symptoms, such as a fingertip sore, your doctor may recommend simply protecting the region and preventing infection.
If your vasculitis is more severe, you may require additional treatment, such as:
- Steroid medicines are given by mouth or through a vein to reduce inflammation
- Immunosuppressant medicines such as rituximab to help control the immune system
- Other immunosuppressant medicines such as cyclophosphamide, if the vasculitis is severe
Your treatment will be carefully tailored to your other health issues and response to therapy by your healthcare practitioner. During a disease flare-up, you may only need to take medications for a brief period of time. However, to control your disease, you may need to take medications for a longer period of time. You may also need treatment for a future bout of vasculitis.
Some of the drugs may have serious negative effects. These include bladder bleeding and an increased risk of infection. Any issues will be monitored by your healthcare practitioner. You may also require treatment to help you avoid the negative effects of your medications. For example, additional calcium and vitamin D may be required to help prevent steroid-induced bone weakening (osteoporosis).
Alternative and Complementary therapies used
when treating Rheumatoid vasculitis patients
Hyperbaric oxygen therapy
For a number of non-rheumatic purposes, Hyperbaric oxygen therapy has been utilised in patients with Rheumatic Disease for many years with no reports of unpleasant or unexpected effects. Hyperbaric oxygen appears to limit the effects of some cytokines, according to new research. Its potential role in rheumatic disorders has been reexamined since it acts as an immune modulator and may assist cognitive impairment 1.
Cryotherapy
Cryotherapy is a non-invasive and rapid technique to make something as complex and life-altering as an autoimmune condition more manageable. It has been shown to lower inflammation produced by many autoimmune conditions, making it one of the most straightforward strategies to begin controlling your symptoms 2.
Ozone therapy
Ozone therapy – Autohemotherapy is still commonly used in Europe and South America to treat chronic pain and inflammation, infections, circulatory abnormalities, fungal infections, acne, eczema, and a variety of other ailments 3.
Red Light Therapy
Although Red light therapy is an excellent symptomatic treatment, it is not a cure. It, on the other hand, does not require injections, medication, or opioids, is painless and is effective at reducing pain, inflammation, and swelling 4, 5.
Infrared Sauna therapy
Infrared sauna therapy can help people with a variety of degenerative conditions, including rheumatoid arthritis, which can cause pain, stiffness, exhaustion, and joint degeneration, among other symptoms 6.

Hyperbaric oxygen therapy
For a number of non-rheumatic purposes, Hyperbaric oxygen therapy has been utilised in patients with Rheumatic Disease for many years with no reports of unpleasant or unexpected effects. Hyperbaric oxygen appears to limit the effects of some cytokines, according to new research. Its potential role in rheumatic disorders has been reexamined since it acts as an immune modulator and may assist cognitive impairment 1.

Cryotherapy
Cryotherapy is a non-invasive and rapid technique to make something as complex and life-altering as an autoimmune condition more manageable. It has been shown to lower inflammation produced by many autoimmune conditions, making it one of the most straightforward strategies to begin controlling your symptoms 2.

Ozone therapy
Ozone therapy – Autohemotherapy is still commonly used in Europe and South America to treat chronic pain and inflammation, infections, circulatory abnormalities, fungal infections, acne, eczema, and a variety of other ailments 3.

Red Light Therapy
Although Red light therapy is an excellent symptomatic treatment, it is not a cure. It, on the other hand, does not require injections, medication, or opioids, is painless and is effective at reducing pain, inflammation, and swelling 4, 5.

Infrared Sauna therapy
Infrared sauna therapy can help people with a variety of degenerative conditions, including rheumatoid arthritis, which can cause pain, stiffness, exhaustion, and joint degeneration, among other symptoms 6.
What are the possible
complications of
rheumatoid vasculitis?
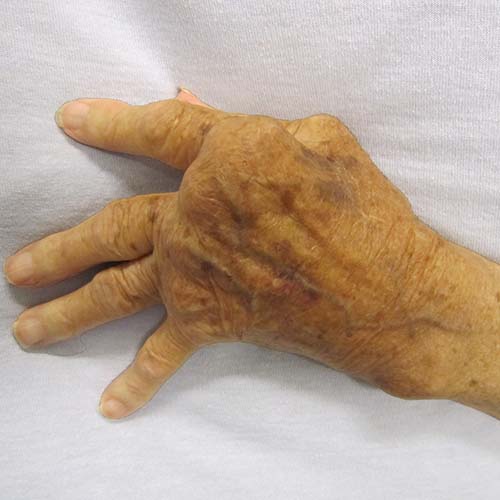
What are the possible complications of rheumatoid vasculitis?
Vasculitis can cause damage to blood vessels in other parts of the body in rare situations. Damage to the lungs, kidneys or digestive tract may result as a result of this.
Vasculitis can cause the following symptoms in certain people:
- Pressure injuries and infection
- Blindness
- Atherosclerosis
- Heart attack
- Inflammation of the sac around the heart (pericarditis)
SUMMARY
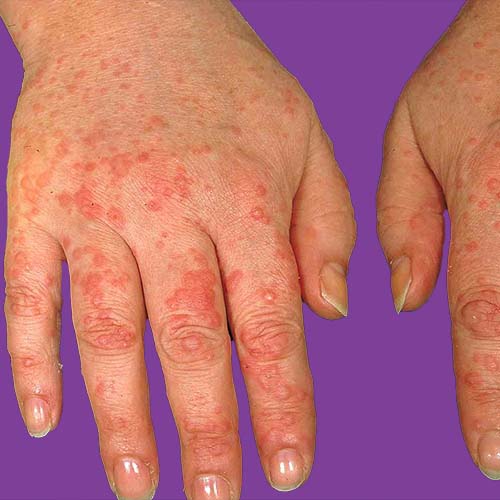
SUMMARY
Rheumatoid vasculitis is a disorder in which small or medium-sized blood vessels become inflamed. It occurs in some persons with RA who have had the disease for a long time.
Skin vessels, fingers and toes, nerves, eyes, and the heart are the most commonly affected.
It can lead to significant problems, including death if left untreated.
During a disease flare-up, you may require steroids and other medication treatment.
Smoking cessation may help you lower your risk.
If you notice signs of a vasculitis flare-up, contact your healthcare professional right once.
Tips for getting the most out of a visit to your healthcare Consultant appointment include:
- Know why you’re coming and what you want to accomplish.
- Make a list of questions you’d like answered prior to your visit.
- Bring someone along to assist you in asking questions and remembering what your provider says.
- Note the name of a new diagnosis, as well as any new medicines, treatments, or tests, during the appointment. Make a note of any new instructions you receive from your provider.
- Understand why a new medicine or therapy has been prescribed for you and how it will benefit you. Also, be aware of the potential adverse effects.
- Check to see if there are any other options for treating your problem.
- Understand why a test or procedure is advised, as well as what the results may imply.
- Know what to expect if you skip the medicine, the test, or surgery.
- Make a note of the date, time, and purpose of any follow-up appointments you have.
- If you have any questions, you should know how to contact your provider.